Basal Cell Skin Cancer
What is Basal Cell Skin Cancer?
Most people are aware of skin cancer. Melanoma, the deadliest type of skin cancer, is by far the most publicized. However, other types of skin cancers exist, and though not usually deadly, they can still be disfiguring and dangerous and must be treated. Basal Cell Carcinoma, referred to by most as BCC, is the MOST common cancer in the world. While Caucasian men over 40 have been known to be more commonly diagnosed with this skin cancer, it is becoming increasingly prevalent among women, as well as for men and women under 40. More than 1 million people are diagnosed with BCC annually, and this statistic increases by 10% every year. This increase is attributed to the aging baby boomer population, an increase in UV light exposure (due to depletion of the Earth’s ozone layer), and a lack of appropriate sun-protective behaviors.
Once one BCC is diagnosed, the risk of developing a second BCC within 5 years is high. Within 10 years 60% of patients will have another non-melanoma skin cancer (BCC or squamous cell). While BCC is enough of a concern on its own, the Journal of the National Cancer Institute also found that those diagnosed with any skin cancer are slightly more likely to have another type of cancer, unrelated to the skin. This risk increases even more in those diagnosed with BCC at a younger age. This information makes it clear that preventing BCC, as well as early diagnosis and treatment of BCC is becoming increasingly important.
Am I at Risk for BCC?
There are many factors that can increase a person’s risk for BCC, including:
- chronic sun exposure
- fair skin type, with red or blonde hair and/or green or blue eyes, or tendency to burn easily and rarely tan (Skin Type l or ll)
- family or personal history of basal cell or other skin cancers
Less common risk factors are therapeutic radiation, chronic immunosuppression – such as transplant recipients or those with HIV – and some rare genetic conditions. The strongest cause of BCC is excessive or chronic sun exposure. UV radiation causes a genetic mutation to several tumor-suppressing genes, which are part of the “hedgehog” molecular pathway (important in early fetal development). The malfunction of those genetic “brakes” allows uncontrolled growth, resulting in basal cell cancer.
The warning signs of BCC include:
- A persistent sore that remains open and does not heal for several weeks
- A red patch, that may or may not be irritated, and that does not go away
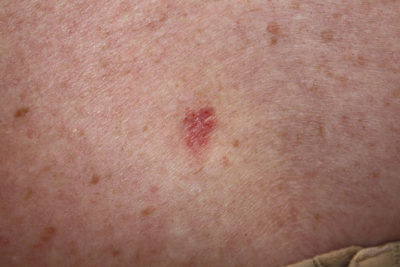
- A new, shiny bump. May be red, translucent, white or pigmented
- A pink, growth with rolled borders and sometimes a central crust. There may also be small blood vessels visible in the growth.
- A white, yellow, waxy area with undefined borders that may look like a scar
The diagnosis of BCC is made after a small skin biopsy has been performed by your dermatologist, which is sent to a dermatopathologist, who then views the tissue specimen underneath the microscope, and analyzes the histology of the cells. At Krauss Dermatology, we use StrataDx’s expert dermatopathologists.
What Do BCC Spots Look Like?
Different types of BCC exist and are important to understand when making a clinical decision about the best treatment option. A nodular BCC is the most common type of BCC and is the case in about 60% of confirmed BCC diagnoses. Nodular BCC appears as a pink, pearly bump that usually has a defined border and may have areas of pigmentation or ulceration.
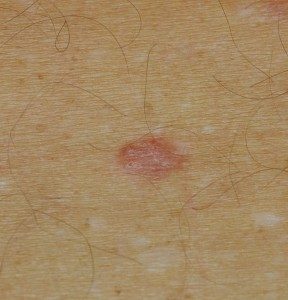
Another common BCC is superficial BCC. These occur in 30% of the cases and are light red and scaly, resembling eczema. An ulcerating BCC is usually firm, translucent, often with a depressed area or crust, and may bleed. A pigmented BCC may be partially or completely brown or blue and has a firm surface that may be depressed. These types of BCC are easy to mistake as melanoma and are found more commonly in people with darker complexions, who naturally have more melanin (the molecule that gives skin its color) in their skin.
Treatment options for BCC are varied and depend on the type of BCC, its location and the patient’s overall health, but are all typically done on an outpatient basis. Higher risk locations for BCC include the areas around the eyes, mouth, ears, and scalp, where there is a risk of cosmetic and functional impairment, and increased risk of recurrence. Foregoing or delaying treatment usually results in extensive damage to the local surrounding tissues, but in extremely rare instances, cancer can metastasize to other organs and tissues.
Electrodesiccation and curettage (a scraping and cautery procedure done in the office) is an option if the BCC is nodular or superficial, smaller than 1 cm, in a low-risk area (such as the trunk, arms, and legs), and is not an aggressive subtype. The malignant tissue is scraped away and electrically cauterized a total of three times in a single visit. This process damages the malignant tissue, leaving surrounding normal skin intact, with a saucer-shaped wound that can take up to 4-6 weeks to heal.
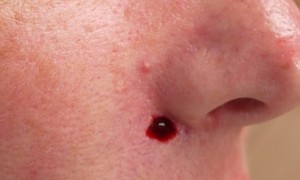
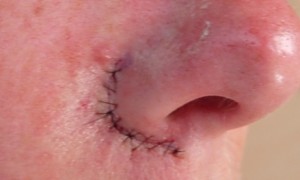
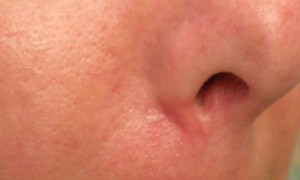
Another option to remove BCCs is surgical excision. A local anesthetic is used, and the malignant tissue is surgically excised with a margin of normal skin tissue around the edges. Sutures (stitches) are used to close the wound. The specimen is then sent for pathology to validate that the margins of the excised tissue are negative. This procedure is best for BCCs that are on the trunk and extremities, for small or mid sized lesions, and if definitive pathology is wanted.
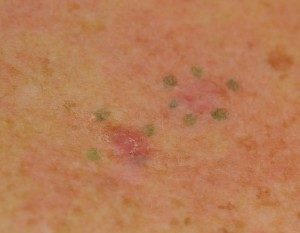
BCC Treatment
Mohs surgery, named after the physician who created it, is a surgical procedure performed by our specially trained dermatologic surgeon, Dr. Suzanne Mosher. This treatment option is best for BCCs with an aggressive growth pattern (determined by pathology), for those in high-risk areas and where removing the least amount of tissue is important, such as the face, or for BCCs of a large size. The Mohs surgeon will remove the visible malignant tissue and look at it underneath the microscope while the patient waits. If there are still malignant cells at the border of the specimen – indication it is not completely removed – the surgeon will go back and remove more and again look at it underneath the microscope. This will be done until there are no remaining, microscopically visible malignant cells. Mohs surgery has the highest cure rate of any procedure for both BCC and for the more worrisome Squamous Cell Carcinoma of the skin.
Other Treatments
Prevention of sun damage is crucial to thwarting a diagnosis of BCC. This means using sunscreen with SPF 30 or higher on a daily basis, applying sunscreens correctly when in direct sunlight (reapplication every 2 hours is important), using appropriate types of sunscreens (UVA/UVB or broad spectrum), avoiding excessive sun exposure whenever possible between 11am and 3pm, seeking shade, wearing long sleeve shirts and wide-brimmed hats, avoiding tanning and burning, and taking vitamin D supplements. Of course, avoiding the use of UV tanning booths is imperative to decrease your risk of BCC, Squamous Cell Carcinoma and Melanoma. In addition, taking Niacinamide, Vitamin B3, 500 mg twice per day has been recently shown to reduce BCC risk by 20% in high risk individuals.
Early detection of BCC will help you avoid more extensive and invasive treatments. Monthly self-skin exams, visting your dermatologist for your regular skin exam, and notifying your doctor of any new or changing lesions are important. Visit http://www.aad.org/spot-skin-cancer for skin cancer information and tips on performing your monthly self-skin exam.
Take the First Step – Request A Consultation
Please fill out the form on this page to request a consultation and one of our knowledgeable medical staff members at Krauss Dermatology will reach out to you promptly. You can also call our Wellesley, MA office directly to schedule – (781) 416-3500.
Krauss Dermatology serves the greater Boston area.
*Individual Results May Vary*

