Eczema
What is Eczema?
Also known as dermatitis, eczema is a group of conditions where the skin becomes INFLAMED—with itching, redness, dryness, or even small blisters in the skin. Itch caused by dermatitis can make us extremely uncomfortable, interrupting our normal daily living, not to mention a good night’s sleep!
What Causes Eczema?
Eczema tends to run in families—it is thought that certain genes can make our skin much more sensitive to outside triggers, or our immune reactions much stronger to these triggers. It also seems that the skin of people with eczema has a harder time retaining its barrier function, which may allow further exposure to outside agents that irritate the skin.
What Are Some Of These Triggers?
- Stress
- Cold, dry weather in winter
- Heat, sweat
- Any product or chemical that comes into contact with the skin
- Clothing, such as wool
Types Of Eczema
The most common type of eczema is called atopic dermatitis, and it affects 10-20% of children and 1-3% of adults. Often described as “the itch that rashes”, it starts with extremely itchy patches of skin, and with scratching they become red, swollen, dry, and sometimes weepy with clear fluid. In infants, these patches are often on the face and scalp, while in children they are most commonly seen at the back of the knee or the inside of the elbow. Some, but not all, children will “outgrow” their condition, with outbreaks (and their severity) lessening with time. Adults with atopic dermatitis may develop areas almost anywhere on the body, with common sites including the eyelids, neck, hands, and feet.
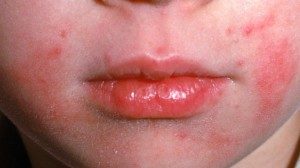
Many parents ask us if their baby or child with atopic dermatitis is reacting to something in his or her diet. Many children with atopic dermatitis also do have food sensitivities and are more likely to have asthma and hay fever. In addition, many atopic children have a high rate of positive reactions with skin testing to foods. It is unclear, however, whether a specific food can directly worsen a child’s skin condition—the two conditions seem to be independent of one another in most cases. As a result, we do not routinely recommend elimination diets or allergy testing in children with atopic dermatitis, focusing instead on the treatment of the skin itself (as detailed below).
Another common type of eczema we see in the office is hand eczema. In an age that (rightfully) promotes frequent hand washing or sanitizing to reduce transmission of germs, all that washing takes a toll on our skin! For some of us, the result is a pair of dry, itchy hands, sometimes with painful cracking. We tend to see this mostly in wintertime, but it can also be a year-round problem, especially in situations where frequent hand cleansing is necessary—i.e. healthcare professions, parents changing their baby’s diaper, etc.
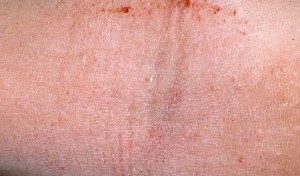
Hand eczema can also develop as a result of an allergic reaction to a product the skin is coming in contact with like soap, shampoo, or moisturizer. When traditional prescriptions and remedies don’t improve hand eczema, Krauss Dermatology offers patch testing to help clarify any possible role skin allergy may be playing in eczema type rashes. Our own Dr. Krauss was interviewed by the Boston Globe about treatment of dry cracked hands, click here to see her recommendations.
Treatments
We’ve discussed a few of the more common types of eczema, as well as what is understood about the condition, but what can be done to treat it?
Hydration of the skin: this is one of the cornerstones of treatment. When the skin is dry and itchy, steps to add moisture and restore the normal barrier function of the skin are a must. A moisturizer in the form of a cream or ointment must be applied frequently, especially after any washing of the skin.
Reduction of inflammation: important for both allowing the skin to heal and for stopping the itch. Topical medications, such as steroid creams, are invaluable to rapidly relieve itching, calm down inflammation and help the skin return to normal. Used for many years in dermatology, topical steroids are extremely safe (even for infants) when used as recommended and for limited periods of time on the skin. Occasionally oral medications, such as prednisone or antihistamines, are also needed if outbreaks are severe. A new injectable biologic agent, Dupixent, has transformed the lives of teens and adults afflicted with moderate to severe atopic dermatitis.
Prevention: once clear, there are often steps that can be taken to prevent (or at least minimize) a future outbreak. When triggers or culpable allergens are known, avoidance of them is certainly important whenever possible. In children with atopic dermatitis, routine moisturizing, especially after bathing, is recommended. In the case of hand dermatitis, limiting hand washing or at least using gentler cleansers followed by application of moisturizers helps prevent flares. When immersing the hands in water (such as washing dishes), wearing gloves is also helpful. Since the skin tends to be dryer in winter, many of us will need to start applying moisturizers in late fall to prevent that dry winter itch from developing.
Eczema is a common condition, one we at Krauss Dermatology see in our patients regularly. While there is no known cure for it, with diligent skin care and effective treatment tailored to each individual’s needs it can at least be tamed so that patients can live as freely as possible from the dreaded itch.

